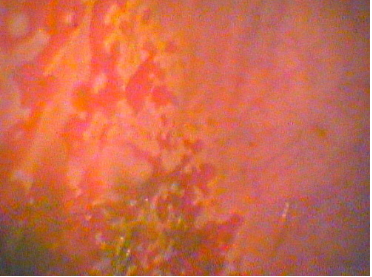
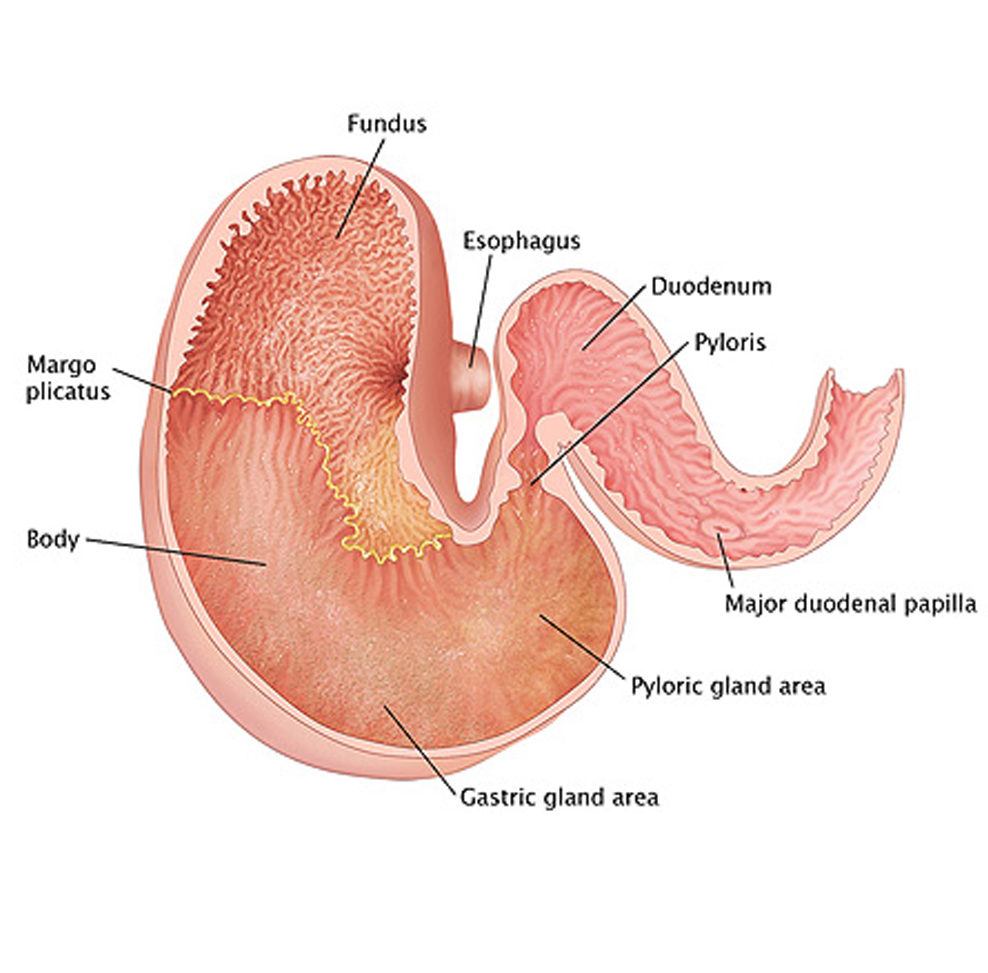
The image above shows multiple ulcers in the non-glandular part of a horse’s stomach. These ulcers bled and show dark red discoloration at each location.
Gastroscopy
3-Meter Video Endoscope
We routinely utilize our gastroscope. The endoscope is long enough to reach into an adult horse’s stomach and the first section of small intestines (the duodenum). This equipment gives us the capability of definitively diagnosing stomach ulcers in horses.
Stomach ulcers are very common in horses in training. Observational studies have shown that up to 90% of horses in training, regardless of breed and type of exercise, may have ulcers of varying severity. Also, the clinical signs shown by horses may not be proportional to the severity of the lesion. The clinical signs are also not always colic type signs, but instead they may be signs such as a poor attitude, poor appetite, poor quality hair coat, or poor performance.
According to Dr. Merritt at the University of Florida, the upper part of the stomach is usually not in contact with ingested food material and especially not in contact with stomach acid. The contraction of abdominal muscles, which occurs during exercise, causes an increase in the intra-abdominal pressure. The increased pressure pushes the acidic stomach content up into the upper part of the horse’s stomach. Repeated exposure to the acid results in ulcers in that portion of the stomach.
Horses at rest in pasture do not experience the increased abdominal pressure of horses at exercise. So, we can understand the association of training with ulcers is not stress related but rather mechanical in nature. We also can understand the importance of checking for ulcers and treating for ulcers if present.
Endoscopy
Optic Endoscope
Our flexible fiber optic endoscope is helpful for evaluating the airway of the horse, including the larynx, sinuses, guttural pouches and trachea. Flexible endoscopy is also useful for diagnosing problems of the bladder and uterus.
Common conditions treated with the help of endoscopy.
Laryngeal hemiplegia
Upper respiratory tract disease
A common disease of horse’s upper respiratory tract. It is commonly referred to as roaring because of the distinctive noise produced by affected horses when they exercise. The disease’s cause is unknown. We know a lot about the epidemiology of the disease and there are several theories about causes.

The disease is much more common in large breed horses, and it is very rare in ponies. Among the large breeds, it affects larger individuals more often, so apparently size is connected to development of the condition. The disease results from loss of nerve function to the muscle that opens the larynx. The larynx needs to open to accommodate for high airflow rates needed during exercise. Importantly, the larynx is the narrowest part of the airway at rest, and it increases in cross sectional diameter more than any other place in the airway. So, when affected by this disease, a horse looses a substantial amount of its ability to inhale an adequate volume of air during exercise. For horses that compete at speed it is a very debilitating disease.
In the picture, Dr. Crawford holds the endoscope in the horse’s nasal passage, while Dr. Martin directs the flexible end toward the horse’s larynx. Disease affecting the horse’s voice box or larynx is a common cause of respiratory noise production during exercise and causes exercise intolerance in athletic horses.
 The picture left was taken through the flexible endoscope showing the characteristics of the disease condition. The first thing to note is the asymmetry of the structure.
The picture left was taken through the flexible endoscope showing the characteristics of the disease condition. The first thing to note is the asymmetry of the structure.
The red outline circumscribes the horse’s right corniculate cartilage, sometimes referred to as the “flapper” because it moves (“flaps”) inward during vocalization and during swallows and outward during exercise. Perhaps more pertinent to the disease is that the cartilage is flaccid and free to flap across the larynx during inspiration. The red line shows the normal position of the right cartilage when the horse is at rest.
Ethmoid Hematoma
Hematoma located the nasal passage
Ethmoid hematoma is a progressive and locally destructive disease of horses. It is indicated by a mass in the paranasal sinuses, that resembles a tumor but is not neoplastic by any means. The origins and causes of the ethmoid hematoma are generally unknown. Large hematoma will usually start within the ethmoid labyrinth, and smaller ones tend to begin on the sinus floor.
The hematoma usually extends into the nasal passage. A growing hematoma causes pressure necrosis of the bone surrounding the hematoma, but only on rare occasions does it cause facial distortion. It is most commonly seen in horses older than 6 years. Mild, persistent, unilateraldeletedsomestuff epistaxis is the most common sign clinically.
Diagnosis of the condition is best suited to endoscopy; the lesion can be seen extending into the nasal passages on endoscopic examination and can be demonstrated on radiographs. Further elucidation can be obtained with MRI or CT in cases which are more widespread or invasive.
Treatment most commonly involves the removal of the complete lesion during a single procedure, via the frontonasal bone flaps; recurrence is likely. Ablation treatment with an Nd:YAG laser looks to be a possibility for permanent removal. There has been some success using intra-lesional injections of formalin, performed via endoscopy.
Arytenoid Chondritis
Inflammation within the larynx
Arytenoid chondritis is a performance-limiting condition in horses. The underlying problem is a primary infection in the body or corniculate process of 1 or both arytenoid cartilages of the larynx. When chronic inflammation or abscessation may deform and permanently immobilize the affected cartilages, partial arytenoidectomy is indicated. Before that point, the process can be arrested by local debridement or drainage of the lesions, which has traditionally been accomplished by laryngotomy with the horse under general anesthesia. Infections of the arytenoid cartilages with granulomas and abscesses can be effectively treated in the standing horse by using the diode laser administered by an endoscopically guided ventral stab incision in the cricothyroid membrane.